Russia’s Sputnik V vaccine, the vaccine that was mocked and ridiculed by American media, has 92% efficacy in trial, scientists say
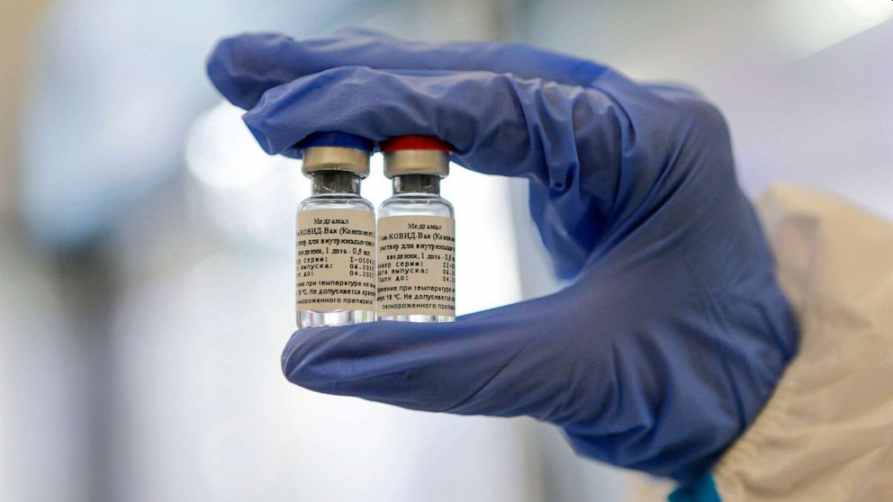
Back in August 2020, we wrote about Russia’s Sputnik V vaccine after the Russian scientists said they have completed the clinical trials of a vaccine against covid-19. The phase clinical trials of the Russian vaccine were completed in less than two months and phase three trials were set to begin shortly.
Russian President Vladimir Putin reportedly said that one of his daughters had been vaccinated against the coronavirus, saying, “In this sense, she took part in the experiment.” Putin said on Tuesday that Russia had become the first country to grant regulatory approval to a COVID-19 vaccine after less than two months of human testing, a move Moscow likened to its success in the Cold War-era space race.
However, within hours of the announcement, American mainstream media quickly piled on the vaccine casting doubt about the safety of the vaccine. Another NBC News article called the decision to roll out the vaccine “reckless and foolish,” adding “whether it works is anybody’s guess.”
Fast forward five months later. According to a report from BBC News, Russia’s Sputnik V vaccine “has also been deemed to be safe – and offer complete protection against hospitalization and death.” According to the report, Russia’s Sputnik V vaccine has 92% efficacy in trials.
“The vaccine was initially met with some controversy after being rolled out before the final trial data had been released. But scientists said its benefit has now been demonstrated,” BBC said.
In a comment published alongside the Lancet paper titled, “Sputnik V COVID-19 vaccine candidate appears safe and effective,” Profs Ian Jones and Polly Roy said:
“The development of the Sputnik V vaccine has been criticised for unseemly haste, corner cutting, and an absence of transparency. But the outcome reported here is clear and the scientific principle of vaccination is demonstrated, which means another vaccine can now join the fight to reduce the incidence of COVID-19.”
The two professors pointed out the vaccine had a good effect on all age groups and reduced the seriousness of the disease after one dose. This was “particularly encouraging” while the supply of the vaccine is limited, they added.
The Russian Sputnik V vaccine was developed by the Gamaleya National Research Center for Epidemiology and Microbiology in Moscow. Unlike Pfizer and Moderna vaccines, the Russian vaccine uses an adenovirus to deliver components of the pathogen that causes covid-19. The approach is similar to one being advanced by Oxford University and AstraZeneca.
The Sputnik vaccine works in a similar way to the Oxford/AstraZeneca jab developed in the UK, and the Janssen vaccine developed in Belgium. It uses a cold-type virus, engineered to be harmless, as a carrier to deliver a small fragment of the coronavirus to the body.
Below is the detailed report.
“Denis Logunov and colleagues1 report their interim results from a phase 3 trial of the Sputnik V COVID-19 vaccine in The Lancet. The trial results show a consistent strong protective effect across all participant age groups. Also known as Gam-COVID-Vac, the vaccine uses a heterologous recombinant adenovirus approach using adenovirus 26 (Ad26) and adenovirus 5 (Ad5) as vectors for the expression of the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) spike protein.
The use of two varying serotypes, which are given 21 days apart, is intended to overcome any pre-existing adenovirus immunity in the population.2 Among the major COVID vaccines in development to date, only Gam-COVID-Vac uses this approach; others, such as the Oxford–AstraZeneca vaccine, use the same material for both doses. The earlier vaccine for Ebola virus disease, also developed at Gamaleya National Research Centre for Epidemiology and Microbiology (Moscow, Russia), was similar, with Ad5 and vesicular stomatitis virus as the carrier viruses,3 and the general principle of prime boost with two different vectors has been widely used experimentally.4
The recombinant adenovirus route to protection is shared with the Oxford–AstraZeneca vaccine, which uses a chimpanzee adenovirus (ChAdOx),5 the Johnson & Johnson vaccine that uses only Ad266 whose detailed results are expected soon, and the CanSinoBIO-Beijing Institute of Biotechnology Ad5-based vaccine whose phase 3 trial began in September, 2020.7
The carrier viruses are modified and cannot initiate a productive infection; they enter cells, express the spike protein, and then stop (because they cannot continue the normal virus lifecycle), although a high-sensitivity analysis also showed that a few Ad genes were expressed, albeit at a low level.8 The vaccine-infected cells are eventually destroyed by the very immunity they are designed to elicit. Recombinant adenoviruses have been used widely as vaccine vectors because they can accommodate large genetic payloads and, although unable to replicate, they trigger the innate immunity sensors sufficiently to ensure robust immune system engagement.9 Consequently, they do not need an adjuvant and can provide immunity after just a single dose.4
Their physical robustness is thought to allow storage at temperatures around –18°C, which is feasible for many supply chains. The downside of recombinant adenovirus-based vaccines is that large doses are required, typically 1010 or 1011 particles, which makes large demands on the manufacturing and quantitation required for rollout on a global scale.
What then of the Sputnik V COVID-19 vaccine data published here? The earlier phase 1/2 data published in September, 2020, showed promising safety results and gave an indication that the immune response was at a level consistent with protection.10 Recipients generated robust antibody responses to the spike protein, which included neutralising antibodies, the proportion of the total immunoglobulin that inhibits the virus binding to its receptor.
They also showed evidence of T-cell responses, consistent with an immune response that should not quickly wane. The interim report of the phase 3 data now presented1 includes results for more than 20 000 participants, 75% of whom were assigned to receive the vaccine, and the follow-up for adverse events and infection. With a planned study power of 85%, those recruited were aged 18 years and older, were about 60% male, and were almost all white.
Comorbidities, a known risk for COVID-19 severity, were present in about a quarter of those who entered the trial. 62 (1·3%) of 4902 individuals in the placebo group and 16 (0·1%) of 14 964 participants in the vaccine group had confirmed SARS-CoV-2 infection from day 21 after first vaccine dose (the primary outcome). A time-resolved plot of the incidence rate in the two groups showed that the immunity required to prevent disease arose within 18 days of the first dose. That protection applied to all age groups, including those older than 60 years, and the anecdotal case histories of those vaccinated but infected suggest that the severity of disease decreases as immunity develops.
Three fatalities occurred in the vaccine group in individuals with extensive comorbidities, and were deemed unrelated to the vaccine. No serious adverse events considered related to the vaccine were recorded, but serious adverse events unrelated to the vaccine were reported in 45 participants from the vaccine group and 23 participants from the placebo group. Vaccine efficacy, based on the numbers of confirmed COVID-19 cases from 21 days after the first dose of vaccine, is reported as 91·6% (95% CI 85·6–95·2), and the suggested lessening of disease severity after one dose is particularly encouraging for current dose-sparing strategies.”